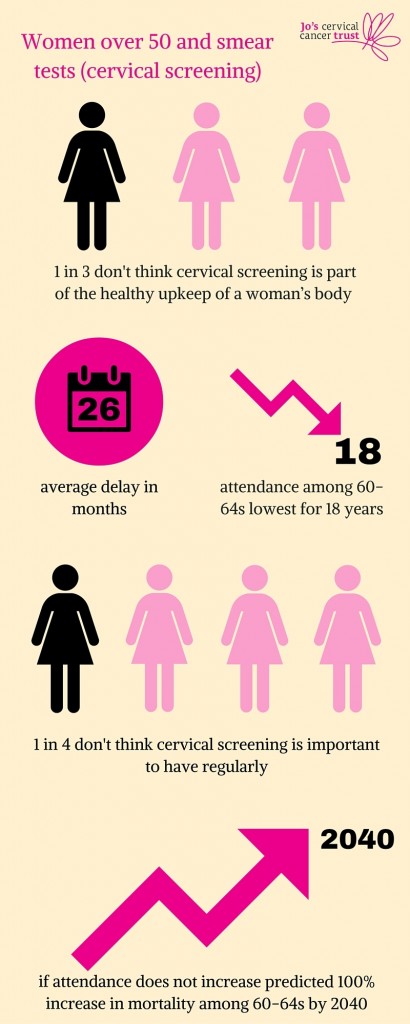
1 in 3 (32%) women over 50 do not think cervical screening (smear tests) are part of the healthy upkeep of a woman’s body and almost 1 in 4 (22%) do not think they are important to have regularly according to new research by Jo’s Cervical Cancer Trust and Gransnet. Adding to concern, a worrying 1 in 3 (33%) have delayed or not attended this potentially life-saving test with an average delay of 26 months and 1 in 10 (10%) delaying for over 5 years.
During Cervical Screening Awareness Week (13-19 June) Jo’s Cervical Cancer Trust, the UK’s only dedicated charity for women affected by cervical cancer and abnormalities, wants to highlight the worrying lack of understanding of cervical cancer and cervical screening among women over 50. Cervical screening provides the best protection against cervical cancer, a disease that can be prevented and the charity wants to see eradicated.
The latest statistics show incidences of cervical cancer in the UK have risen from 8 diagnoses every day to 9 each day meaning 3,207 women a year now face a diagnosis. Adding to concern, new modelling work commissioned by Jo’s Cervical Cancer Trust has uncovered a ticking time bomb: incidences of cervical cancer are set to rocket if current uptake of cervical screening remains the same.
By 2040 incidences will have increased by 16% among 60-64 year olds and 85% among 70-74 year olds. A 100% increase in mortality among 60-64 year olds is also a very real threat rising to a massive 117% if screening uptake continues to decline and falls by another 5%.
Further findings from the survey of over 1,000 women aged over 50 found:
- Almost half (46%) do not agree or do not know the Human papillomavirus (HPV) (the cause of almost all cases of cervical cancer) is common
- 1 in 5 (21%) do not agree or do not know that regular cervical screening reduces the risk of cervical cancer
- Of those who have delayed screening, 32% find it embarrassing, 25% find it hard to book an appointment at a convenient time, 20% have had a previous bad experience and 19% find it painful since being older (16% since the menopause in particular)
When asked what would encourage attendance:
- 21% said more flexible GP opening hours
- 38% said being sent an appointment time with their cervical screening invitation
- 31% wanted more information relevant to their age
- 23% said more information about the risks of not attending
- Almost 1 in 4 (23%) who had delayed attending said the opportunity to HPV self test
Robert Music, Chief Executive, Jo’s Cervical Cancer Trust: “Cervical cancer is a preventable disease so it is extremely worrying that diagnoses have risen. Women aged 50 to 64 are of particular concern as they are more likely to receive an advanced stage diagnosis, with 49% of diagnoses stage two or later, which means more invasive treatment, poorer health outcomes and increased risk of loss of life.
“Not attending cervical screening is the biggest risk factor to developing cervical cancer, yet attendance declines with age and among women aged 60-64 uptake is now at an 18 year low at just 72.4%. Relevance, accessibility and flexibility are significant barriers to cervical screening among this group and coupled with our modelling work, which shows terrifying long term increases in incidence and mortality among this age group, it has never been more crucial that we act.
“For women who are post-menopause, screening can be particularly uncomfortable, and our research shows discomfort (57%), mild (26%) or even severe pain (10%) are common screening experiences. Further research into HPV self-sampling tests is urgently needed as it could help overcome some of these barriers for this age group. The 2015 Cancer Strategy for England highlights the need to increase screening attendance and I am afraid that if we do not tackle this with a sense of urgency we are only exacerbating the ticking time bomb of increased incidence.”